- More than 60% of Australians will receive a diagnosis of skin cancer before the age of 70.
- More than 2000 Australians are dying of skin cancer each year.
- More than 2,500 skin cancer treatments occur in Australia every day.
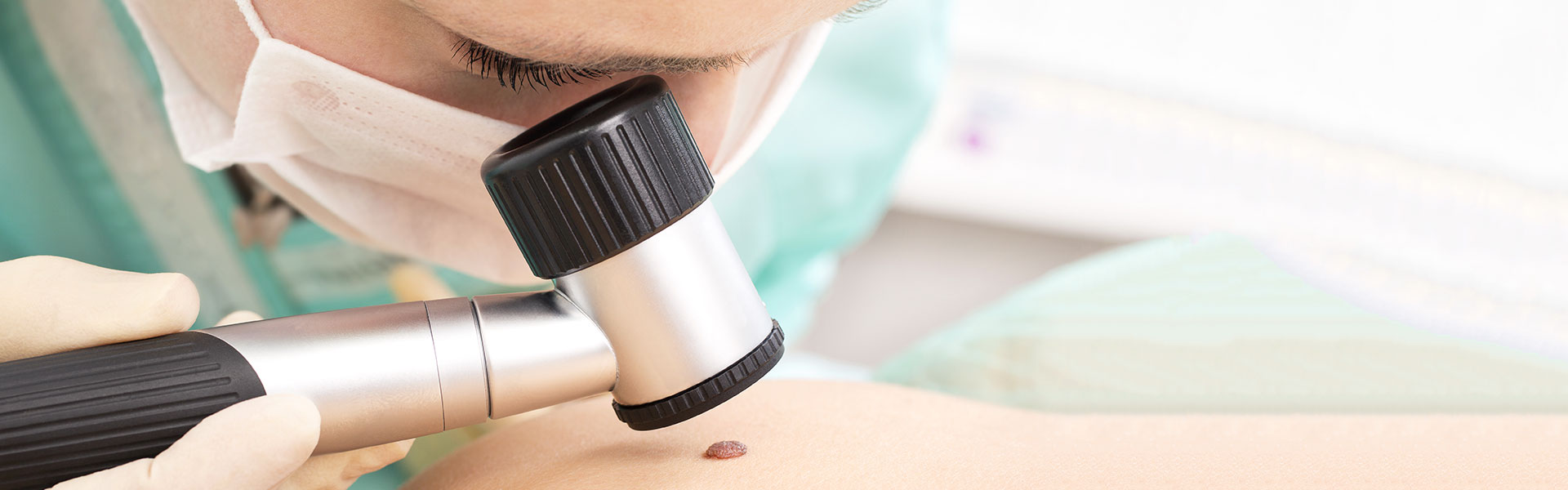
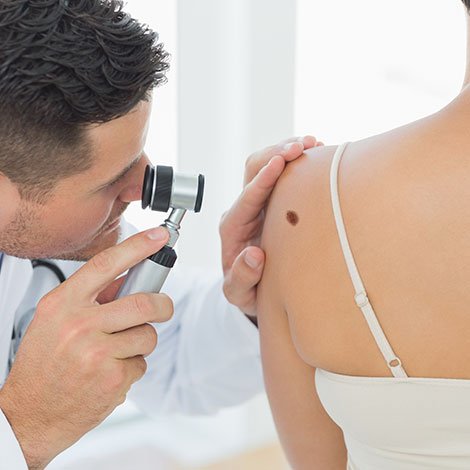
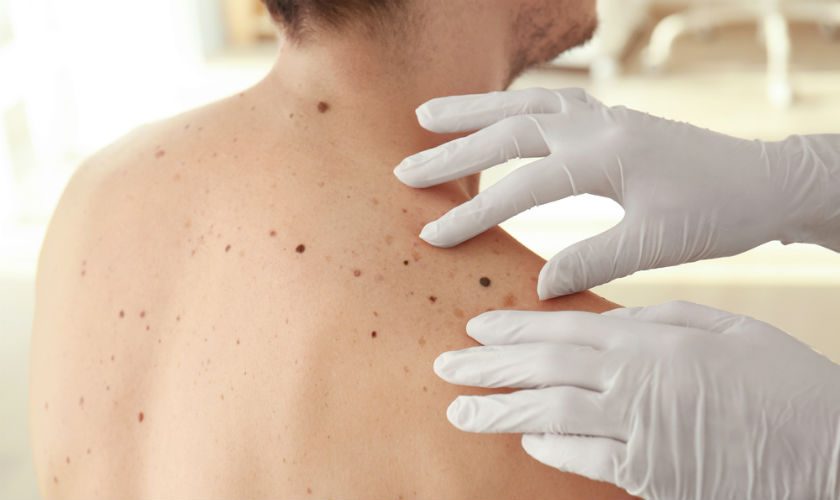
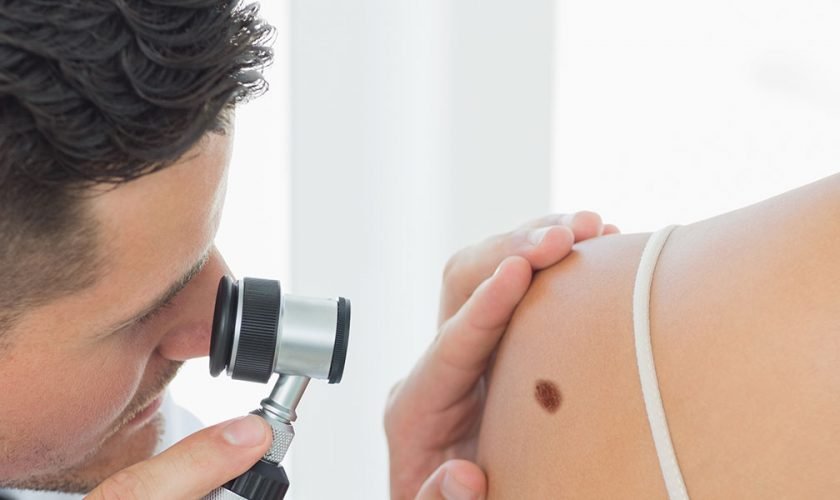
A professional skin check could save your life. If a patient’s cancer is detected early during a routine scan, their prognosis is promising, with their condition likely to be more treatable than a person whose skin cancer scan may have been done too late.
One of the most advanced methods of early skin cancer diagnosis is to get a detailed, full body skin check in Melbourne combined with full body mole mapping. For a comprehensive mole check, mole removal or follow-up imaging, make an appointment at Mole Check Clinic.